Hot Flash! Menopause May Not Be Sexy, But Investors Are Warming To Digital Health Solutions
Executive Summary
The menopause market is a multi-billion opportunity that is gaining traction with digital health companies offering innovative solutions to help women manage their symptoms and provide treatment and support. Medtech Insight spoke with three female founders and entrepreneurs, as well as a partner at Lux Capital and the clinical lead of ORCHA, about this niche market.
Menopause is a $600bn market opportunity that remains largely untapped, according to the Female Founders Fund. But a growing field of digital health solutions including telemedicine, digital therapeutics and women’s health apps, are striving to address this growing market.
With an estimated 1.1 billion women worldwide being postmenopausal by 2025, innovators and investors are starting to pay attention to a market that has long been overlooked.
“It’s a space that has been ignored for years due to social stigma, a fragmented health care system, and under-investment in women’s health care,” said Alessandra Henderson, co-founder and CEO of health tech company Elektra Health.
Deena Shakir, partner at venture capital firm Lux Capital, also sees the perimenopause and menopause space as a “massive opportunity” for start-ups to provide innovative solutions for employers seeking to attract and retain talent – “especially amidst the ‘Great Resignation.’”
“It’s a space that has been ignored for years due to social stigma, a fragmented health care system, and under-investment in women’s health care.” – Alessandra Henderson
“Employers and payers are increasingly interested in benefits focused on women’s health, but there has been limited investment in innovation addressing menopause specifically,” Shakir told Medtech Insight.
It’s an area where unconscious biases – sexism and ageism – persist.
“It’s also an area where differentiation has been hard to achieve, especially given limited innovations in therapeutic interventions. Many D2C approaches have required heavy upfront investments in user acquisition and marketing, which can be challenging for some to translate to venture scale,” Shakir added.
Fatima Ahmed, a practicing obstetrician and gynecologist who is the clinical lead at the UK-based Organisation for the Review of Care and Health Applications (ORCHA), said while existing telemedicine and app solutions offer women access to good, digitized information and virtual consultations with clinicians, which saves travel time and can also expedite treatment, she’d like to see more solutions that fulfill needs beyond access.
ORCHA has reviewed hundreds of femtech apps and health care apps to provide transparency and guidance for patients, health care professionals and organizations, and governments, taking into account such factors as data security, clinical assurance, and user experience.
“Even if they are not addressing all accessibility because a lot of these solutions are expensive, cost money, and are only available in the English language, but they are at least trying to bridge that gap of different barriers to seeing a clinician and [can] help more people on a bigger scale than a clinician sitting in their office,” Ahmed said.
Many women start experiencing menopause between the ages of 45 to 55, ultimately resulting in loss of fertility and periods. In the transition to menopause, called perimenopause, many women develop symptoms including hot flashes, night sweats, anxiety, depression, mood swings and sleep problems.
According to the AARP, only 20% of OB-GYN residency programs in the US offer menopause training and 80% of medical residents admit they feel “barely comfortable” discussing or treating menopause.
A 250-women survey conducted by the Female Founders Fund to better understand the overall needs of women through menopause found that only 36% of respondents felt “moderately or very prepared” for menopause; 32% believed that their health care providers are not knowledgeable or confident to discuss menopause.
Ahmed noted that in the UK, patients often have a long wait time to get face-to-face with a menopause specialist, which are in short supply.
“It’s actually hard to find somebody who is a menopause specialist. Particularly if the menopausal symptoms are more troublesome than the usual presentation, or ones that are more challenging to treat … the more complex cases will take a really long time to be seen by the right person, which is tragic, because it can really ruin lives,” Ahmed told Medtech Insight. Adding to the problem is that general practitioners, often the first stop for menopausal women seeking clinical advice, don’t often have a good understanding of the issue, which can lead to misdiagnosis of symptoms.
One company that is trying to tackle that problem is Bia Care, which was incubated by Zinc VC, the UK’s largest social impact accelerator, and Kamet Ventures, the leading health tech venture builder, and is backed by Atomica Angels. The virtual group consulting model connects patients to doctors in small groups to increase availability of clinicians and avoid long wait times that are common with other providers of menopause care.
Rising Investment
Investments in start-ups focusing on the perimenopause and menopause segment are gaining traction. According to Rock Health, which tracks US digital health start-ups who have raised $2m and above in venture capital since 2011, such companies raised a total of $88.48m in 2021 – still a tiny fraction relative to the $29bn raised in overall 2021 digital health funding.
Digital behavioral health start-up Happify Health, which offers the Kopa platform supporting menopausal women, topped the funding list with $118.3m raised, followed by Evernow ($28.5m), Embr Labs ($12m), Joyl ($11m), G ($4m), Elektra Health ($3.7m), Alloy ($3.3m), Aveta.Life ($2.48m) and myLAB Box ($2.27m).
Elektra Health
Elektra Health’s Henderson said while the women’s health tech has raised slightly over $4m in total funding in a pre-seed and seed round, she recalled that during her 30-minute pitches to investors, she spent more time educating investors on the menopause space than talking about the opportunity.
“We got definitely our fair share of ‘nos’ – over 90 ‘nos’ for a seed round – but we persisted and we found the people who believed in us from the beginning,” Henderson told Medtech Insight. Last August, Elektra closed a $3.75 million seed round, co-led by Flare Capital Partners and Seven Seven Six, a new venture firm started by Reddit co-founder Alexis Ohanian, with participation from City Light Capital, January Ventures, Human Ventures, the Fund, Company Ventures, the Community Fund, and others. The funding will be used to expand Elektra’s team and its digital platform, which brings together education, care and community.
The company has a paid subscription platform where women can book telemedicine visits with a gynecologist and nurse practitioner in Florida, Connecticut, New Jersey and New York.
It also offers virtual wellness consultations and sexual health consultations. Henderson said seed funding will help accelerate development of a paid subscription program called “Meno-morphosis” that provides ongoing community support and text-based support from a dedicated expert for women going through menopause.
The program starts with an assessment where the woman is asked about her symptoms and what is important to her, then pairs her with a registered nurse to develop a wellness plan. The program is in beta testing, but is expected to debut later this year, Henderson said. Pricing has not been set, but Henderson expects annual subscription costs between $50 and $250.
“Our biggest goal is to make something accessible to women who are in need of ongoing support,” she said.
Since Elektra’s founding in 2019, it has built a community of more than 17,000 members. The Meno-morphosis platform has several hundred founding community members. Henderson noted that while the telemedicine visits are currently only available in four states, the digital platform and guide support from menopause experts will be available nationwide.
Henderson said the idea for Elektra came out of her personal journey with hormonal health back in 2017 when she froze her eggs and the hormones from egg-freezing later impacted her eyesight.
“I just fell down the rabbit hole of research and hormonal health,” she said. After talking to numerous experts and women going through hormonal changes, she determined there was a lack of information and stigma surrounding menopause.
“Women told me that they felt invisible,” she said.
With her own background in consumer technology and building brands, having worked for the New York City-based online art brokerage Artsy and serving as executive director for the MIT NYC Startup Studio, Henderson co-founded Elektra with Jannine Versi, who spent over a decade working in health tech, tech and government, and Anna Barbieri, a gynecologist at Mount Sinai School of Medicine in New York.
Among the more recent fundraising success stories is Evernow, founded in 2019 by Alicia Jackson and Aaron Gotwalt. Evernow announced in April it raised $28.5m in series A funding to provide virtual 24/7 menopause support, including access to hormonal therapies.
The round was led by global capital firm NEA with participation from 8VC, Refactor Capital, and Coelius Capital, as well as Hollywood celebrity investors Gwyneth Paltrow, Drew Barrymore and Cameron Diaz and powerful executives like Morgan Stanley’s Carla Harris and Care.com founder Sheila Marcelo.
Vira Health
In March, London, UK-based start-up Vira Health, which offers the digital therapeutic Stella designed to support women going through menopause, raised $12m from lead investor Octopus Ventures with participation from US venture firm Optum Ventures and existing investors. That built on a $2m seed round last summer, backed by LocalGlobe, MMC, Amino Collective and angels. The money was used to build the first version of Stella, a lifestyle and behavioral change app for menopause.
Andrea Berchowitz, Vira Health’s co-founder and CEO, told Medtech Insight, “It [Stella] combines all of the best digital apps out there … whether that’s a sleep app or a pelvic floor-focused app or a mindfulness app … If they [women] are struggling with the symptoms of menopause, we provide the guidance that they need to make the lifestyle, behavior, exercise, nutrition changes to help them manage their symptoms … We also create a community that supports one another, a place for expert answers to questions they [women] might have, and hopefully also a little bit of humor, because sometimes that’s necessary.”
The company plans to use the new funding to build on the app’s care pathway, adding a telemedicine component that will allow users to virtually consult with a physician and get prescriptions, such as hormone replacement therapy. Berchowitz said Vira Health completed a feasibility study in early 2022 and expects to “kick off the next step in that process in the first quarter of 2023.”
Founded in 2020 by Berchowitz, who previously spent almost 11 years at McKinsey & Company where she consulted on women’s health issues and one year at the Bill and Melinda Gates Foundation heading Middle East relations, and Rebecca Love, a chronic disease epidemiologist and expert in behavior change, Vira Health seeks to fill a gap in menopause care, which is personalized support to help women manage their specific symptoms.
“What we’ve built is something that flexes to a woman-specific symptom situation – the woman who is dealing with incontinence and weight gain will have a different plan than the woman who is dealing with sleep issues and feelings of anxiety,” Berchowitz explained.
The Stella app, first introduced in the UK last August and now also available in the US, offers a 12-week program that comprises complex guidance around lifestyle and behavior change via weekly lessons.
“It [Stella] combines all of the best digital apps out there … whether that’s a sleep app or a pelvic floor-focused app or a mindfulness app … If they [women] are struggling with the symptoms of menopause, we provide the guidance that they need to make the lifestyle, behavior, exercise, nutrition changes to help them manage their symptoms." – Andrea Berchowitz
Berchowitz explained that a woman with incontinence symptoms may receive a program that includes daily pelvic floor activation or core-strengthening exercises while a woman with sleep problems may receive support on decreasing caffeine intake and sleep scheduling to create better sleep habits.
Each program is based on the best science available for the symptom, drawing on best practices, she said. But the app is not currently regulated as a medical device; rather, it is offered as an information service. Adding a telemedicine component will require regulatory clearance, but Berchowitz doesn’t foresee any issues on that front.
“The regulatory path in telemedicine is much clearer now. Pre-COVID it was probably more complex, but now, so many companies offer telemedicine that the complexities I think are well traveled, so it’s not something I’m worried about.”
The app also allows users to interact with experts and communities through group coaching sessions, exercise classes, and work with nutritionists.
“We’ve chosen our plans to be 12 weeks because we feel that is enough time that things start to bed in a little bit, but we can’t expect people to check an app every single day forever,” she said. Most women choose to focus on another symptom once they finish the first 12-month program, she said.
Berchowitz declined to say how many users its app has at this stage. Vira’s business model is two-fold. Direct-to-consumer paid subscriptions – £20 ($24.95) monthly and £70 ($87.32) yearly – and a B2B2C approach through an employer or a benefits platform employers work with, which is broadly the approach for marketing the app in the US.
“Most women on our platform have come through either their employer or a benefits platform,” she said. “We think that workplaces providing high-quality benefits and care … really need to consider menopause in their offer, and we’re starting to see some uptake on that, especially in the UK.”
Ahmed also deems it important to make digital health technologies part of the health care system so these solutions become subsidized for patients.
“That’s why it becomes important for organizations like ORCHA working with health-care systems, helping them implement these digital technologies, and really driving forward that proper use of digital health technologies and creating a proper infrastructure, so they can be offered in the NHS (National Health Service) like drugs and people don’t have to pay for them,” she said.
Among other notable apps that seek to help women learn about and manage menopause symptoms is Caria. Founded by Arfa Rehman and Scott Gorman, who met at Oxford University during their graduate work, Caria’s approach combines self-guided cognitive behavioral therapy techniques with nutritional science and physical exercise.
‘Good’ Apps
Happify’s Kopa app, which offers women in midlife information and access to a sympathetic community as well as medical professionals, met ORCHA’s baseline review standards across the three main components of data security, clinical assurance and user experience. Another app, Balance-Menopause support, also scored high by ORCHA’s standards and is already included the ORCHA App Library.
Ahmed noted that ORCHA scores apps based on their “trustworthiness,” but leaves it up to the clinicians to decide which digital therapeutic best meets the needs for their patients.
“We build the infrastructure to allow the safe delivery of good apps and also improve accessibility to good apps,” she said. Ideas among innovators differ as to what makes an app good. Berchowitz said Stella is designed to provide personalized support based on what the user tells them they are most concerned about. But it doesn’t require the user to log symptoms.
“We find that women actually find symptom-logging and that sort of tracking quite anxiety-inducing, and so that’s not how we approached it,” she said.
“If a woman is dealing with hot flashes and night sweats, she knows that and whether it’s seven or 10 isn’t the point. If it’s disruptive, then focusing on ways to reduce that disruption is what matters.”
IdentifyHer
IdentifyHer co-founder Heidi Davis, on the other hand, says her company’s approach is rooted in symptom-tracking. The Ireland-based company is using AI-enabled technology to collect objective data via a wearable biosensor that can be used by clinicians to personalize the management of menopausal symptoms and treatment plan.
Davis told Medtech Insight that about 75% of all women in the menopausal transition, including perimenopause, suffer moderate-to-severe symptoms that can make their life difficult. Of the 60% of women that seek help, only 30% will get treated, leaving 70% of women tolerating symptoms.
“We want to really try and bridge that gap between the clinician that doesn’t have a diagnostic test to establish perimenopause and the woman that doesn’t understand what she’s going through and wants treatment,” Davis said.
Self-reporting symptoms doesn’t provide a clinician with an accurate picture of frequency and severity of symptoms, which is what IdentifyHer’s companion diagnostic tool in development is meant to achieve.
Ahmed said the idea of a wearable to track symptoms “in principle sounds very good,” because it would give the physician critical clinical data early on, which helps streamline care by allowing clinicians to spend more time with their patients discussing treatment options.
“We want to really try and bridge that gap between the clinician that doesn’t have a diagnostic test to establish perimenopause and the woman that doesn’t understand what she’s going through and wants treatment.” – Heidi Davis
The data could also potentially be used to show patients, who have already started treatment, if they are responding to treatment or not.
“You can really just skip to the main points [during an office visit] without having to possibly waste time looking at things that aren’t important,” Ahmed said. “It will essentially provide you more targeted clinical time, especially where our time is so limited.”
Formally established in October 2021, IdentifyHer started with €50,000 from Enterprise Ireland, a government agency responsible for supporting Irish businesses, and partnership with sensor company Analog Devices, which developed the prototype for initial data collection. IdentifyHer is currently raising seed funding of €2.2m, which it hopes to close in October.
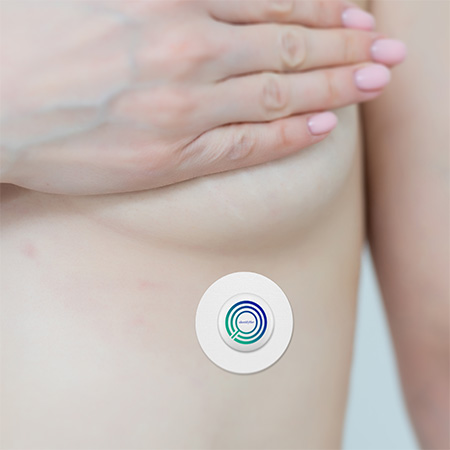
The IdentifyHer rechargeable wearable biosensor sits under the woman’s left breast, which Davis said is the location on the body where researchers were able to detect physiological changes accurately enough to build the algorithms. The device is designed to be worn for up to three months to provide clinicians with enough information to develop a treatment plan, and will be activated by an app. The wearer goes about her normal daily activities and will get daily, weekly and monthly reports on menopausal symptoms, which can be shared with the clinician who can upload the data remotely.
The business model is B2B2C where the company will partner with digital health platform companies that will use their wearable AI to guide the diagnoses and management of menopause. Customers will be menopausal specialist clinics to start with and then primary health care facilities that will supply the trackers to patients, she said.
At this time, the tracker is still in development, but Davis hopes to gather a critical mass of proof-of-concept data to launch the product in late 2023, pending regulatory clearance. The company is using the prototype to collect data on 100 women, who are logging symptoms of hot flashes and night sweats for three days.
“It’s really to build our algorithms and strengthen the ones we have [to detect symptoms of hot flashes and night sweats] as well as to expand into sleep quality and anxiety,” Davis explained. The trial is being run by the Health Innovation Hub Ireland.
The tracker, which will be used to guide diagnosis, will likely be a Class II medical device and will require a CE mark in Europe and eventually FDA clearance. IdentifyHer will rely on its partnerships to develop the final product and take it through the regulatory process.
Davis says that while competitors offer supplements or “cooling” wearables such as the Embr Labs Wave, designed by MIT graduates, or Grace developed by UK femtech start-up Astinno to lower body temperature with targeted cooling sensations on the inner wrist, she claims that IdentifyHer is the only company that provides objective data on menopausal symptoms.
When it comes to prescribing digital technologies, Ahmed acknowledged that we shouldn’t be using technology for technology’s sake, but leveraging it as another solution in managing patient care. It shouldn’t be forced on patients and also shouldn’t be used to marginalize already underserved populations, thereby widening health care inequalities.
“Just be careful with technologies that we don’t forget what their purpose is for and that they don’t replace existing models of care and existing ways that we interact with patients, because that’s still very important,” she said.